Mission
Our mission is to improve Vermonters' health and well-being by providing access to high-quality, cost-effective health care.
Our mission says that we are striving to improve Vermonters’ health and well-being. We provide access to high-quality health care. We are committing to doing this cost-effectively. We are accountable to our members, providers and to taxpayers.
To support our mission, we:
- Help Vermonters access health insurance through Medicaid and through the Health Insurance Marketplace, Vermont Health Connect.
- Help Vermonters who are covered by Medicaid access health care services.
- Pay health care providers for delivering health care to Vermonters who are covered by Medicaid.
- Spend taxpayer dollars wisely by running an effective, efficient department.
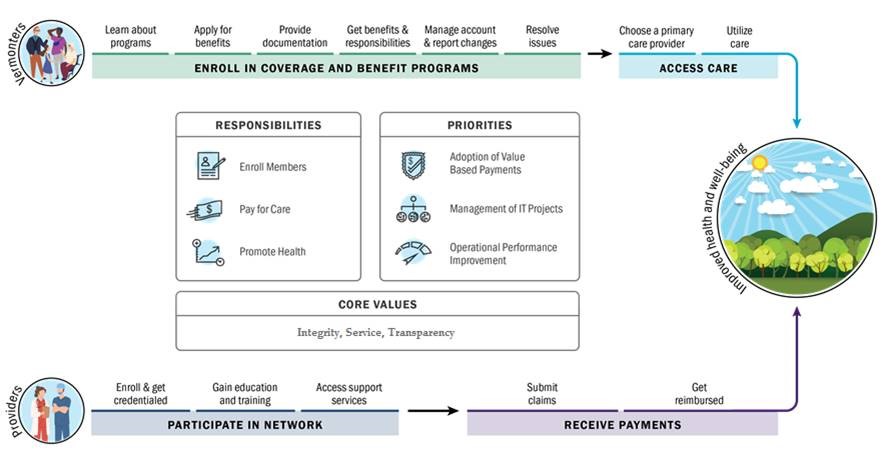
Core Activities
- We encourage Vermonters to sign up for, or enroll in, health insurance and benefit programs. This work is represented by the “Vermonters” path in the diagram above.
- We pay for Vermonters’ health care if they are in Medicaid programs. We work with a robust network of health care providers, pharmacies, and other partners. The Department does not pay for health care for Commercial insurance nor Medicare insurance.
- We strategically invest in programs and monitor costs. This work is central to our commitment to quality and improvement.
Values
Our department follows three core values:
- Transparency – We trust that we will achieve our collective goals most efficiently if we communicate the good, the bad, and the ugly with our partners and stakeholders.
- Integrity – We are ethical and honest. Our actions align with our core values as employees of the Department and of the State of Vermont.
- Service – Everything we do is funded by taxpayers to serve Vermonters. Therefore, we must ensure that our processes and policies are person-centered. We aim to model, drive, and support the integration of person-centered principles throughout our organizational culture.
These values guide our pursuit of our responsibilities, priorities, and mission. We are committed to innovation and collaboration. We approach opportunities to manage Medicaid costs differently with an open mind and are committed to serving Medicaid members, providers, and Vermont taxpayers. We recognize that the success of our initiatives depends on strong working relationships with other state agencies, federal and local governments, and community partners.
Priorities and Connection to the Mission
DVHA has identified three key priorities that support our mission to improve Vermonters’ health and well-being by providing access to high-quality, cost-effective health care.
Advancing Value-Based Payments
Value-based payment programs pay for Medicaid-covered health care in a new way, resulting in predictable and flexible payments for providers and for DVHA, as well as quality of care for Medicaid members. Instead of paying providers solely for the number of services they deliver (e.g., for each test, office visit, hospital stay, and procedure), value-based payment programs link payment to quality, pay differently, or do both. If the value-based payment program pays differently, it can be for entire or selected populations of patients. AN important element of value-based payment is regularly monitoring cost, coordination, volume, and quality of care to support all Medicaid members having access to the services they need.
Modernizing Information Technology Infrastructure
Health care and health insurance systems rely on technology. Vermonters and providers need modern, effective technology systems to sign up for health insurance, to be paid for health care services, and to get the health information they need. Our goal is to implement and use flexible, responsive information technology systems in the face of changing customer expectations, a shifting federal landscape, and advances in the healthcare industry. Modern, effective technology solutions support signing up for health insurance, paying health care claims, and accessing health information.
Operational Performance Improvement
Continuous improvement is a core tenet of the Department’s work. To improve, DVHA staff determine meaningful ways to measure our work, gather data and develop scorecards to monitor effectiveness. These scorecards drive clinical initiatives, business decisions, the pursuit of better customer service, a higher quality of care, and operational efficiencies.
